 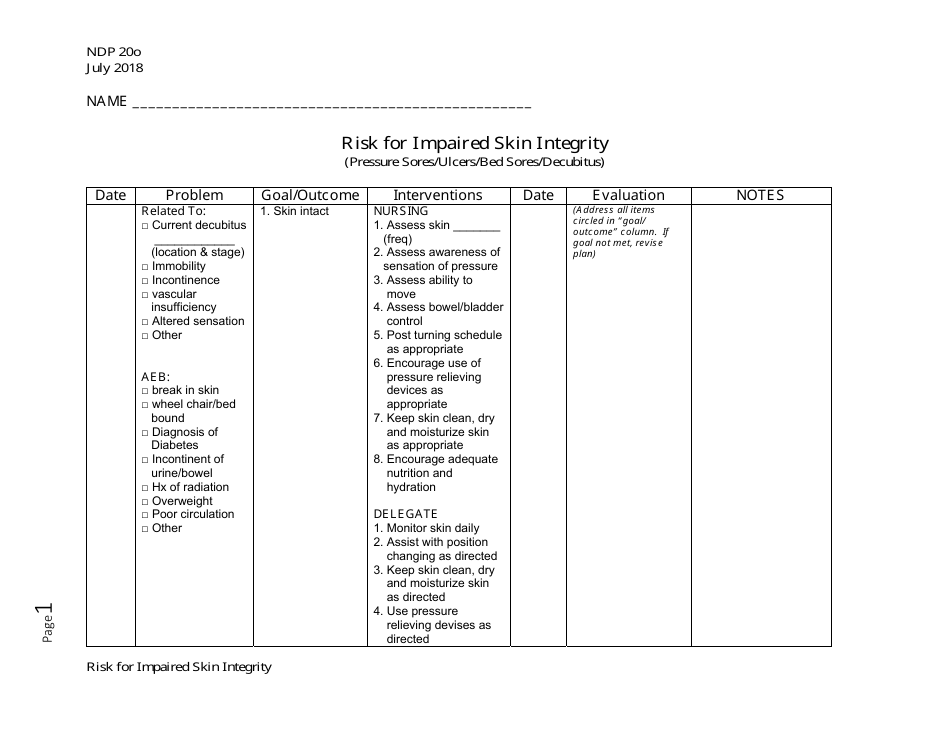
Diabetic, hyperglycemic rats were found to have inferior biomechanical properties than euglycemic rats after injury. The biomechanical properties of diabetic skin are another critical aspect of wound-healing physiology. 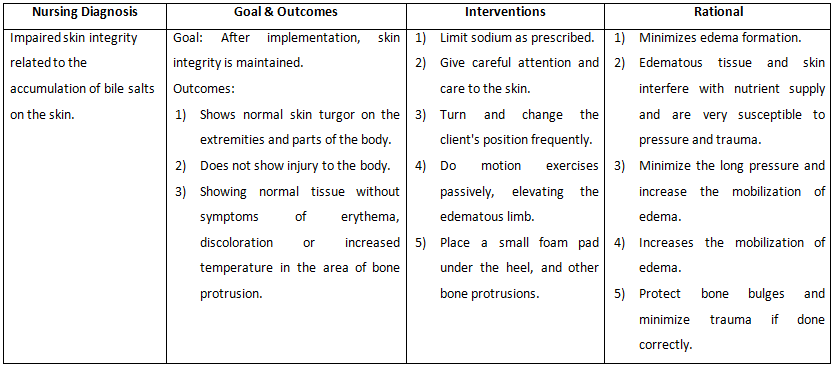
9,13 Furthermore, diabetic (Db/Db) mice have also been shown to have a prolonged inflammatory phase with sustained expression of the inflammatory cytokines macrophage chemoattractant protein 1 (MPC-1) and macrophage inflammatory protein 2 (MIC-2). 12 Hyperglycemic animals have been shown to have significantly higher concentrations of glycated collagen and higher levels of collagenase activity. 10,11 Blockade of the receptor for advanced glycation end products (RAGEs) can restore the wound healing properties of diabetic (Db/Db) mice. 9ĭiabetes is characterized by significantly increased cross linking and nonenzymatic glycation of collagen, as well as elevated levels of advanced glycation end products (AGEs). MMP-2 and MMP-9 have been shown to be present in greater concentration in wounded diabetic animals than their nondiabetic littermates, which is similar to findings from patients with nonhealing ulcers. 3 Decreased angiogenesis, 4 impaired growth factor production, 5 an altered inflammatory and immune response, 5 a decreased rate of wound contraction, 6 and an imbalance between the accumulation of extracellular components and their remodeling by matrix metalloproteinases (MMPs) 7,8 have all been demonstrated in diabetic wounds. More than 100 factors have been identified that contribute to the impairment in diabetic wound healing. 
2 Improvements made in diabetic wound management and prevention clearly have the potential to affect a large number of patients and decrease diabetic-related health care expenditures. 2 Diabetes-related admissions accounted for 22% of all hospital inpatient days in 2007, and diabetic foot ulcers account for 20% of all hospital admissions in diabetic patients, which are the leading cause of lower extremity amputations. These findings suggest that the predisposition of diabetics to wounds may be the result of impaired tissue integrity at baseline, and are due, in part, to a defect in the regulation of collagen protein synthesis at the post-transcriptional level.ĭiabetes is associated with increased morbidity and mortality, 1 as well as impaired wound healing. Collagen I levels and I:III ratios were lower in diabetic skin ( P < 0.05). In addition, MMP-2 and MMP-9/TIMP-1 protein ratios were significantly lower in murine diabetic skin ( P < 0.05). Surprisingly, the expression of genes involved in collagen synthesis were significantly up-regulated, and genes involved in collagen degradation were significantly down-regulated in murine diabetic skin ( P < 0.01). At baseline, both murine and human diabetic skin was biomechanically inferior compared to nondiabetic skin, with decreased maximum stress and decreased modulus ( P < 0.001 and < 0.05, respectively). Collagen I and III content was assessed using Western blot analysis. MMP-2 and MMP-9, and TIMP-1 protein levels were assessed by ELISA and zymography. Real-time PCR was performed for genes integral to collagen synthesis and degradation. Skin from diabetic and nondiabetic mice and humans underwent biomechanical testing. We hypothesize that diabetic skin possesses inferior biomechanical properties at baseline, rendering it more prone to injury. Diabetic skin is known to have deficient wound healing properties, but little is known of its intrinsic biomechanical properties. 
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
